Pulmonary Barotrauma (PBT) through the experience of HMC Sharm el Sheikh
The HMC Sharm el Sheikh has treated hundreds of diving accidents over the years yet, compared to cases of decompression sickness or other pressure related injuries such as otic barotrauma, PBT remains an uncommon diagnosis among the cases presented to the centre. One explanation for this is that cases of PBT can pass asymptomatic or undiagnosed due to a vague clinical picture or association of a more aggressive disorder that masks the cause. In some cases, the unavailability of investigative facilities or lack of time due to severity of symptoms might not allow the clinician to investigate the presence of a possible PBT.
PBT occurring during ascent is relatively more common than PBT of decent, which is often called “lung squeeze” and famous among free/breathhold divers. In this article, PBT of ascent will be our concern.
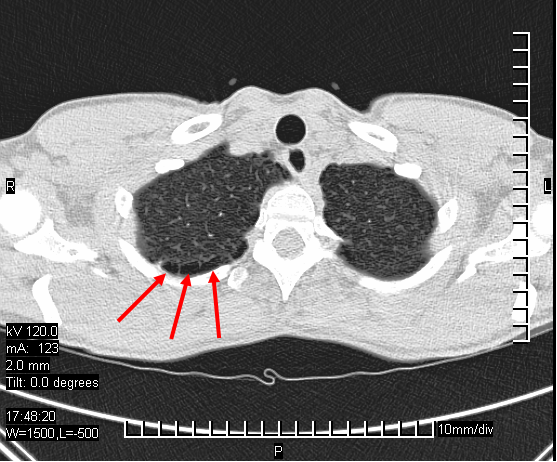
Bullae in the lung
Let's start by refreshing our memory of PBT definition, commonly named lung over expansion injury. It is a condition where exposure of the lung to a gas pressure gradient beyond its compliance will lead to a tissue damage and possible leakage of air. Going back to Boyle's law, one can understand the mechanism of the disorder from a physical perspective. This condition is likely to occur due to divers holding their breath during ascent after breathing gas at depth or due to a condition that prevents venting (or expiration) of gas from lungs such as obstructive lung diseases or due to an existing weak point on the lungs e.g. bullae or scarring.
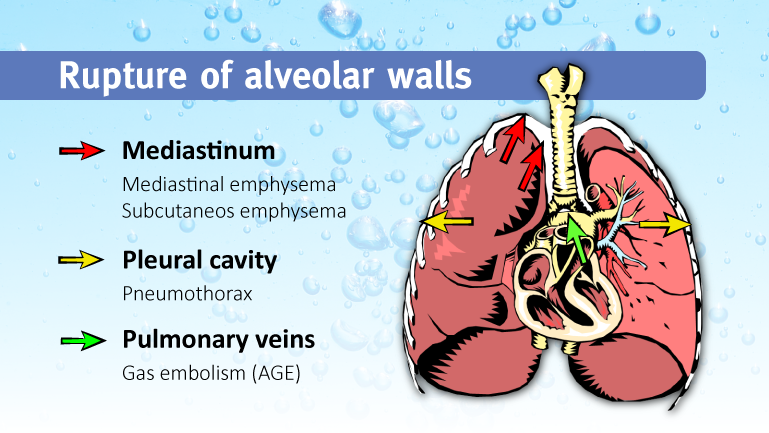
Leakage of the air from the lungs can present in different ways, depending on the anatomical location. Leakage of air into the chest cavity will cause a pneumothorax, if it leaks into the pericardium, a pneumo-pericardium or mediastinal emphysema can occur. If air leaks under the skin, it will cause surgical emphysema. Gas embolism occurs when air leaks into the blood vessels.
Hence, conditions or diseases that impede flow of air leaving the lung or causing air trapping may pose a serious health hazard to a scuba diver, spontaneous pneumothorax cases, active asthmatics, cavitating lesions and emphysema, and COPD cases. There are reports of PBT of ascent occurring in free or buoyant ascents as in submarine escape training which is not a common practice in recreational diving.
PBT of ascent occurs among recreational divers who have pre-existing lung diseases whether obstructive, neoplastic, granulomatous or congenital. Our centre also received cases of PBT caused by heavily straining under water while working on a mooring line or retrieving heavy objects. It is also worth noting that PBT is a different disorder and is caused by a different mechanism than pulmonary oedema, which is caused by immersion or exhaustion (swimmers lung oedema), where body fluids permeate into the alveolar space and impede gas exchange through the alveolar wall precipitating dyspnea, blood tinged expectoration and respiratory distress.
Case report
We chose a case for this article with a non-classic history and two concomitant conditions that may precipitate gas embolism to demonstrate the clinical difficulties in diagnosing PBT.
History
A 33 year-old male diving instructor with experience (> 600 dives) presented to our facility in 2013. Shortly after a single 27.4 msw dive for 45 minutes using compressed air in the Red Sea, he suffered acute paraparesis and disturbed conscious level. He was brought to HMC (Hyperbaric Medical Center Sharm el Sheikh) by Search and Rescue on oxygen. The dive performed was non-eventful without any clear precipitating factor, no difficulty in equalization, coughing or straining, no fast ascents or strong currents, and the safety stop was correctly executed.
Examination at our facility
Clinical findings were as follows: Blood pressure 140/90 mmHg, pulse 114/min, SpO2 93% room air, RR 22/min, pale. The patient reported retrosternal chest pain and there was audible reduced air entry on the lungs associated by generalized coarse crepitations.
Neurologically, patient was drowsy and irritable, reduced sensation from mammary line to feet and severe para paresis, more pronounced on right lower limb, absent superficial abdominal reflexes, knee and ankle hyper-reflexia, positive Babinksi's, positive clonus, stool and urine retention.
The past medical history was interesting since the victim showed symptoms after a dive on a liveaboard earlier the same year. He had performed a single morning dive on air to 35 msw for around 50 minutes. Most of the dive was in the shallow and no deco stops. After 15 minutes through the dive and during ascent, at 2msw, he felt awkward and felt pressure in his chest when climbing on the boat. After a few seconds, he started feeling dizzy and generalized weakness set in. He was provided oxygen and the symptoms gradually resolved. He refrained from diving until end of safari. On return to his country, the instructor had a PFO scan, which came back positive grade 1 shunt, and upon consulting a diving specialist over there he was cleared to resume diving and the incident was blamed on the PFO.
Back to the actual case
At our centre, the patient was diagnosed with a gas embolism and recompressed quickly to a USNTT6, which was repeated over the following 2 days and later HBO sessions were given. He was hospitalized for close medical monitoring and catheterization and received physiotherapy.
Investigating the cause was commenced and on a plain posteroanterior chest X-ray view, an approximately 5cm round cavity in the left upper lung was noted. Blood work was non-particular, brain and spine MRI were performed showing no abnormality, (follow-up CT/MRI would have been useful).
Due to the unavailability of full-scale investigations, an aspirate of the abscess was not obtainable, however, a sputum analysis was performed and came back positive for gram-negative bacteria of Klebsiella.
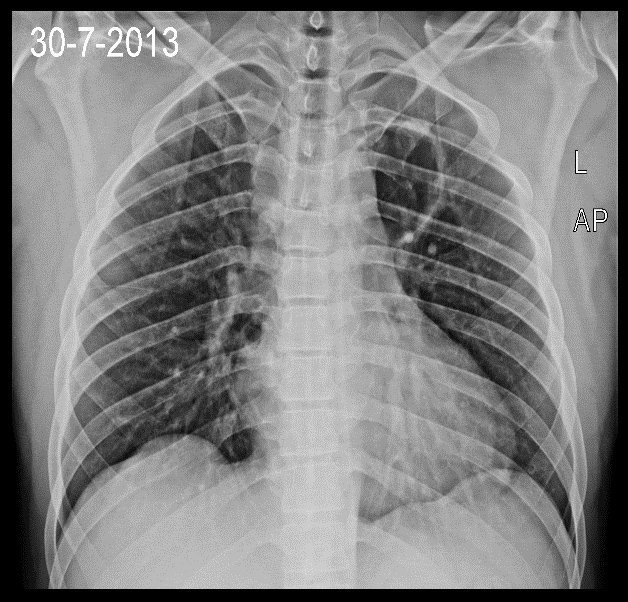
Round cavity left upper lobe.
Outcome
The patient showed slow progressive in-complete recovery and was left with residual weakness in the legs and foot, he was able to walk with crutches, with faint reduction in sensory perception over the dorsum of feet bilaterally, sphincter control was regained. Further treatment was continued at his home country after his departure.
Conclusion
Analysing this case with presentation of a severe neurological injury of the central nervous system following gas embolism, one is left in confusion whether the PFO or the lung cavity or both should be blamed. It is logical that the two post dive incidents are related to an embolic lesion, and it could have been that the cavity was there at the time of first incident.
There is a tendency to point the finger towards the cavity as on the first incident, the patient felt pressure in his chest and on the second incident he reported retrosternal chest pain, which increased, on inspiration and this would be more possible with air in the chest cavity more than a case of PFO.
Cavitating lung lesions are not an uncommon report in tropical and subtropical countries; in Egypt, we see cases of tuberculous and amoebic lung abscesses, which would be no surprise as Entamoeba Histolytica infection is common in touristic areas and other areas as Egyptian delta. Diving instructors or divers are usually the travelling type and mostly visit tropical and subtropical countries.
Treatment of such cases will require multiple approach intervention, recompression therapy besides critical care, pulmonology care and psychological support which poses quite a burden especially in remote areas with limited access to a certain level of investigative facilities or specific specialists. Recompression therapy is only indicated in case of gas embolism consequent to the PBT, while treatment of the cause can be decided electively when the patient is fit to undergo an additional medical intervention.
Accordingly, urgent and rapid treatment of the associated neurological complications remain a priority to treating the cause, and the rate of deterioration of condition can sometimes prevent the clinician from taking the time to conform an etiological diagnosis which can be performed at a later stage.